Transcatheter Aortic Valve Implantation
Background
The aortic valve is the exit point for blood being pumped out of the heart to the rest of the body. If the aortic valve becomes damaged, usually due to calcification, this can result in what is known as “aortic stenosis”, or narrowing. Narrowing of the aortic valve limits the amount of oxygenated blood reaching vital organs, particularly when the body is working harder. In cases of severe aortic stenosis, it is necessary to replace the aortic valve with a prosthetic valve.
Definition
In the past, aortic valve replacement would require open-heart surgery to access the heart and aortic valve. New surgical techniques have been developed to allow for a less invasive approach. Now it is possible to implant a prosthetic valve inside the native heart valve via a procedure called “TAVI or “Transcatheter aortic valve implantation”. This new technique allows the surgeon to gain access to the heart without opening the chest. This kind of surgery is considered suitable for patients with high risk of complications from the open procedure.
Procedure
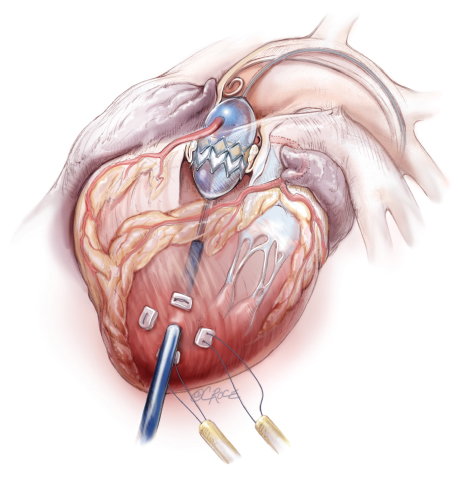
There are ongoing technological advances in the design of the prosthetic valve itself. It is now available in a unique contractible-expandable form. This allows the contracted valve prosthesis to be mounted onto a wire device and fed through a smaller access site to the heart. Once it is in the correct position, the valve is expanded to fit correctly inside the native heart valve and left in place. There are two main options for gaining access to the heart in this new minimally invasive procedure. These are the “transapical” and “transfemoral” approaches. The transapical approach (i.e. “through the apex of the heart”) involves making a small incision in the chest, just below the left nipple and accessing the apex of the heart directly. The valve prosthesis is fed through the left ventricle of the heart to reach the aortic valve. The transfemoral approach involves making a small incision in the groin and feeding the wire device up through the aorta until it reaches the heart. The surgeon is guided by x-ray and ultrasound imaging to see the position of the device. Once it reaches the correct position, the surgeon deploys the prosthetic valve, so that it expands and fits within the patient’s own aortic valve. After the procedure, the patient is transferred to the intensive care unit where he or she is monitored and supported in the post-operative period.
Benefits
TAVI has been tested against medical therapy in nonoperative patients and open aortic valve replacement in high surgical risk patients. This procedure has shown promising benefits including
- Increased survival when compared with medical therapy for non-operative patients
- Improved quality of life
- Minimally invasive advantages compared with the open surgical approach for high-risk patients • Transapical approach allowing direct access to the heart, especially for patients with severe peripheral vascular disease, which limits access through the groin vessels
Risks
Potential complications associated with the procedure include
- Bleeding and clotting at surgical incisions
- Stroke and myocardial infarction
- Pericardial effusion/tamponade (fluid/blood collecting around on the heart)
- Risks associated with the transfemoral approach and related to the vascular access site, such as bleeding, infection and femoral artery damage
- Death
Suitability
It is a matter of weighing these risks against the benefits. This analysis will be different for each patient, taking into account both the individual risk profile as well as the potential for an improved quality of life. TAVI is currently used only in elderly and high-risk patients whose risk profile prohibits them to undergo surgical aortic valve replacement. At this stage, the long-term results of TAVI are unknown. Future trials may focus on lower risk patients. Please consult your cardiologist and cardiac surgeon for professional advice.
For more information, please visit the following websites:
http://guidance.nice.org.uk/IPG421/Guidance/pdf/English
http://www.ctsnet.org/sections/clinicalresources/clinicalcases/article-28.html
Services
Cardiac Surgery
- Aortic Arch Surgery
- Aortic Stenosis
- Aortic Surgery and Stroke
- Aortic Valve Repair
- Coronary Artery Bypass Grafting
- Heart Failure
- Tissue and Mechanical Heart Valves
- Type B Aortic Dissection
- Ventricular Assist Devices
- Hybrid Aortic Arch Surgery
- Marfan Syndrome
- Minimally Invasive Aortic Valve Replacement
- Minimally Invasive Atrial Fibrillation Surgery
- Minimally Invasive Mitral Valve Surgery 2015
